Our Services
Preventive dentistry is the practice of caring for your oral health including your teeth. The goal is optimum oral health and preventing problems like
- Cavities
- Gum disease
- Enamel wear and more.
Initial Consultation / New Patient Check Up
The first people you will meet will be our friendly reception staff, who will ask you to complete a medical form.
Our dentist needs to be aware of your general state of health as this can often impact upon the condition of your teeth and gums and may effect medication such as anaesthetics and antibiotics we may use for you.
At your consultation you will have the opportunity to discuss any dental concerns you may have or how you would like your teeth improved.
Your dentist will give you a full oral assessment to help accurately plan which treatments would be best for the health of your mouth.
During this examination we will be looking at -
Teeth and the way you bite, plus any missing teeth
Original restorations – fillings, crowns, veneers etc.
The health of your gums and surrounding bone around each tooth
Your tongue, throat, cheeks and lips for signs of change from the normal
Dental X-rays
Dental X-rays will also be taken of your teeth to check for -
Decay inside the tooth or between the teeth.
Abscess or cysts on the roots of your teeth.
Root positions
Bone loss
Once the examination is complete, we will discuss the findings with you.
We will then create a treatment plan with alternative options for you, including all the benefits and risks of each procedure and the costings. This will allow you to decide what is best for your long term dental health.
Panoramic Dental Xray - OPG
Panoramic dental x-ray uses a very small dose of ionizing radiation to capture the entire mouth in one image. It is used to plan treatment for dentures, braces, extractions and implants. It is an invaluable tool to view impacted wisdom teeth and their proximity to nerves.
This exam requires little to no special preparation. Tell your dentist if there is a possibility you are pregnant. You will be asked to wear a lead apron to protect the rest of your body from any radiation exposure. Remove any jewelry, eye glasses or metal objects that might interfere with the x-ray images.
Periodic Examination / Reviews
The best way to maintain good oral hygiene is to brush and floss your teeth and to visit your dentist for regularly. Your dentist not only examines your teeth for signs of decay or damage, he also looks for early signs of gum disease and oral disease.
It is normally recommended that you visit your dentist twice a year, although people who have severe gum disease or a weakened immune system may need to visit the dentist more often

Veneers
Veneers are thin layers of material that cover the front of the teeth and are designed to improve their appearance. While veneers can improve your teeth’s appearance, poorly fitted veneers can cause jaw pain.
Veneers can be made either of porcelain (ceramic) or composite resin (of plastic and glass)
Porcelain veneers tend to look more realistic and last longer than resin veneers, but they are also more expensive
Veneers are a permanent dental treatment, and their colour cannot be altered after they’ve been applied.
When might someone want veneers?
Veneers are generally used to improve the appearance of teeth
rather than to repair damage.
You might choose to have veneers on your teeth if they are:
discoloured or stained
crooked, oddly shaped or chipped
Veneers can only be applied if your teeth and gums are in good condition.
They may not be suitable if you grind or clench your teeth because that can
crack the veneer.
What happens during a dental veneer procedure?
Porcelain
Your dentist will first remove a thin layer of enamel from the tooth so that
the veneer does not stick out. You might be given a local anaesthetic for
this procedure. The dentist will then take an impression of the tooth. The
mould is sent away to a lab where the veneer will be made.
In the meantime, your dentist can give you a temporary veneer. During your second visit, the dentist will make sure the veneer fits well and that it looks good. The bonding cement is then set using a beam of light.
Composite
A composite resin veneer is completed in one visit. The dentist applies the
material to the tooth in layers, each hardened using a beam of light.
Finally, the tooth is shaped and polished. But it shouldn’t be painful.
What to expect after a dental veneers procedure?
Your dentist may ask you to come back so they can check your gums and how
the veneers are sitting.
You should treat your veneers in the same way you do your regular teeth
by:
practising good oral hygiene
brushing and flossing daily
avoiding biting hard or chewy food (or chewing your fingernails) because
veneers can chip
What are the benefits and risks of choosing veneers?
Using dental veneers is a fairly simple approach that can significantly improve the look of your teeth, if that’s what you want.
teeth whitening:
What is teeth whitening?
Teeth whitening involves bleaching the teeth to lighten their colour. After
treatment, the teeth look a few shades whiter, but not usually bright white.
Teeth whitening is an optional procedure — it is very rarely a necessity.
When might someone need teeth whitening?
If you are considering teeth whitening, you should consult your dentist to see if your teeth are suitable.
Teeth whitening is not recommended if you:
are pregnant or breastfeeding
have sensitive teeth
have gum disease or shrinkage
have cracks or exposed dentine
Note that whitening treatments will not whiten existing crowns, veneers or
fillings.
What happens during a teeth-whitening procedure?
Bleaching
Your dentist will first create moulds of your top and bottom teeth. These
are used to make customised trays, like a mouthguard, that fit over your
teeth.
At your next appointment, bleaching gel is put into the trays, which you
wear in your mouth for 15 to 30 minutes. The dentist might also shine a
light to speed up the whitening process. Often, the treatment is repeated at
home, following the dentist’s instructions. You’ll probably notice a
difference in 2 to 4 weeks.
Another option is to get a kit with the customised trays from your dentist
and carry out the treatment at home.
Can my toothache go away on its own?
Some toothaches that come from pain around (but not inside) your tooth can get better without a trip to the dentist. Pain from a temporary irritation (redness) in the gum can be resolved within a few days. During this time try not to chew around the affected area. Eat soft foods, like eggs and yogurt, and avoid sweets and very hot or very cold foods if teeth are sensitive.
How will the dentist treat my toothache?
Treatment by a dental professional depends on what is causing your toothache.
If a cavity is causing the toothache, your dentist will fill the cavity or take the tooth out, if necessary.
A root canal (a procedure to remove and replace infected pulp with sealing material) may be needed if the cause of the toothache is an infection of the tooth's nerve. Bacteria that have worked their way into the inner space of the root of the tooth cause infection.
An antibiotic may be prescribed if there is fever or swelling of the jaw. A small piece of food (like a popcorn hull) can get stuck under the gums causing an infection. In this instance, a deep cleaning may be performed or recommended followed by further periodontal (gum) therapy if necessary.
Teeth may have to be extracted if they are damaged beyond repair.
Can a toothache make me sick, or even be fatal?
A toothache itself isn’t fatal. But an untreated infection in your tooth (or any other part of your body) can spread. You can become sick, and this illness could turn into something serious or even life-threatening. So if you toothache isn’t getting better it’s a good idea to contact your dentist
Oral surgery and extractions
Oral Surgery including extractions, are surgical procedures that are sometimes necessary to restore oral health and function, this includes soft and hard tissue surgery.
We provide a range of oral surgery procedures including single or multiple tooth extractions, wisdom teeth surgical removals and implants.
Dental Extractions
Dental Extraction is the removal of a tooth from the mouth. It is performed for a wide variety of reasons.
Tooth decay – If the decay is severely advanced and the nerves and blood vessels in the tooth have been infected, and are unsuitable for root canal treatment.
Impacted wisdom teeth – Sometimes our mouths are simply not big enough to accommodate these teeth. The teeth become impacted (stuck), this can cause infection and pain.
Orthodontics (braces) – Teeth can erupt in many different positions, if this happens you may have to have teeth extracted so your other teeth can be brought into line.
Periodontal disease - Bacterial infection under the gum damages the tissue which connects the tooth to the gum; as the disease progresses, the bone anchoring the tooth to the jaw begins to dissolve, resulting in the tooth becoming loose.
Fractured teeth damaged by trauma
Certain medical conditions may require teeth to be extracted.
Your dentist will examine your tooth and explain the reasons why your tooth needs to be extracted. An x-ray will be taken to help plan the best way to remove the tooth.
If an abscess is present your dentist might give you a course of antibiotics before your tooth is extracted.
Your dentist will ask you about your medical history. You must list every medication you are taking even if you have purchased it from over the counter, as some medications can complicate an extraction
Tell your dentist if you are anxious about the procedure as we maybe able to prescripe medication to help manage your anxicty.
Make sure you had something to eat before the extraction.
How the extraction is carried out
There are two types of extraction - simple extractions and surgical extractions.
A simple extraction is performed when the tooth can easily be seen in the mouth. The dentist will give you a local anaesthetic to numb the area around the tooth. When the anaesthetic has taken effect and the area around the tooth is numb, the dentist will hold the tooth using a pair of forceps, you will feel pressure but NO pain. The dentist will move the forceps back and forth to loosen the tooth in order to extract the tooth.
A surgical extraction is carried out on teeth which
Cannot be seen in the mouth but are present below the gum.
Partially showing through the gum
Broken off at gum level.
A local anaesthetic will be administered to numb the area before a small incision is made in the gum. The gum is pulled back to expose the whole of the tooth or the root. The dentist then uses the same procedure as a simple extraction to remove the tooth. In some cases, the tooth or root may have to be divided into pieces to be removed.
When the tooth has been removed, you will be asked to bite on clean cotton gauze until the bleeding has stopped and a blood clot has formed.
Wisdom Teeth
Adults have up to 32 teeth, of which four are wisdom teeth and these are the last to come through the gum. They are the one's right at the back of the mouth and usually appear between the ages of 17 and 25 although sometimes they can appear in later years.
If there is enough room in the mouth the wisdom teeth will come through (erupt) in a useful position and there will only be minor discomfort as they erupt. However, wisdom teeth can cause problems if there is not enough room in the mouth, as the wisdom tooth erupts at an angle and gets stuck against the tooth in front; the dentist will describe this as 'Impacted'.
The dentist will be able to assess whether there is sufficient room for the teeth to come through by taking an x- ray which will show the position of the root. Once the x-rays have been taken, the dentist will be able to tell how easy or difficult it will be to remove the tooth. The dentist will then determine whether the tooth should be taken out at the Dental Practice or by a Specialist Oral Surgeon.
Do I Have To Have My Wisdom Teeth Removed?
The dentist will only recommend taking out wisdom teeth if -
The teeth are not able to fully erupt through the gum and are causing an infection in the surrounding tissue; this is known as Pericoronitis, or
The large nerve supplying the jaw is going to be jeopardised in the future
There is decay present - wisdom teeth will often decay as it is very difficult to clean them as thoroughly as your other teeth.
Following the removal of wisdom teeth, there is likely to be some discomfort. However, this will vary depending on how difficult it was to remove the tooth. It is not uncommon to experience some swelling and/or bruising for a few days.
The dentist will advise on how best to reduce this discomfort and may recommend pain killers such as Paracetamol or Ibuprofen. A further dental appointment will be necessary for the dentist to check the healing process and remove any stitches
Root Canal Treatment
This dental procedure is carried out when the innermost part of the tooth ‘the pulp’ becomes badly decayed or infected. If left untreated, the tooth will begin to die which could lead to the loss of the tooth. To save the tooth, the infected pulp needs to be removed to prevent the formation of an abscess. In dental terms this procedure is called ‘Endodontics’.
After a root canal is successfully done, a porcelain crown should be considered, as this will help prevent the tooth from fracturing. This is especially helpful if a large restoration was originally done, with not much tooth structure left to work with.
Fillings:
What is a dental filling?
A dental filling is a procedure used to fill a hole, or cavity, in a tooth. You may need a filling if you have tooth decay or if the structure of the tooth is lost due to trauma. These problems may be found when you have a dental x-ray.
What types of filling are there?
Various materials can be used as fillings. Your dentist will usually advise you which is suitable for you.
Amalgam
Amalgam has been used for more than 150 years. It is a mixture of metals, including silver, copper, tin, mercury and zinc, and is a very strong filling material. Although exposure to mercury can be toxic, amalgam is safe and effective to use for most people. You can choose not to have amalgam fillings - tell your dentist.
Composite resin
Composite resin is a white or tooth-coloured material. It can be matched to the colour of the other teeth and looks more natural than amalgam, but it is a bit more expensive. Some studies have suggested it might not last as long when used to fill adult back teeth, where there is a lot of pressure.
Glass-ionomer cement
Glass-ionomer cement can also be matched to tooth colour, but it might not last as long as composite resin. It is usually used in areas where there is not much biting force and on baby teeth.
Temporary fillings
If there is not time to finish treating a tooth, the dentist may suggest a short-term temporary filling. This will be replaced by a permanent filling at a later date.
What to expect after a filling
After a filling, the affected tooth might feel sensitive when you eat something sweet or bite your teeth together, or when the temperature changes. You should see your dentist if this continues.
What are the benefits and risks of a filling?
A filling is usually a simple, early treatment for tooth decay and it might make the tooth sensitive for a short time. Over time, fillings may chip or crack, allowing food to become trapped between the tooth and the filling. However, a dentist will usually check your fillings during a regular dental check-up.
What are the alternatives to a dental filling?
Sometimes a dentist may use a crown rather than a filling. A crown fits over the tooth to protect its structure, and may be used if there is not enough tooth left to support a filling
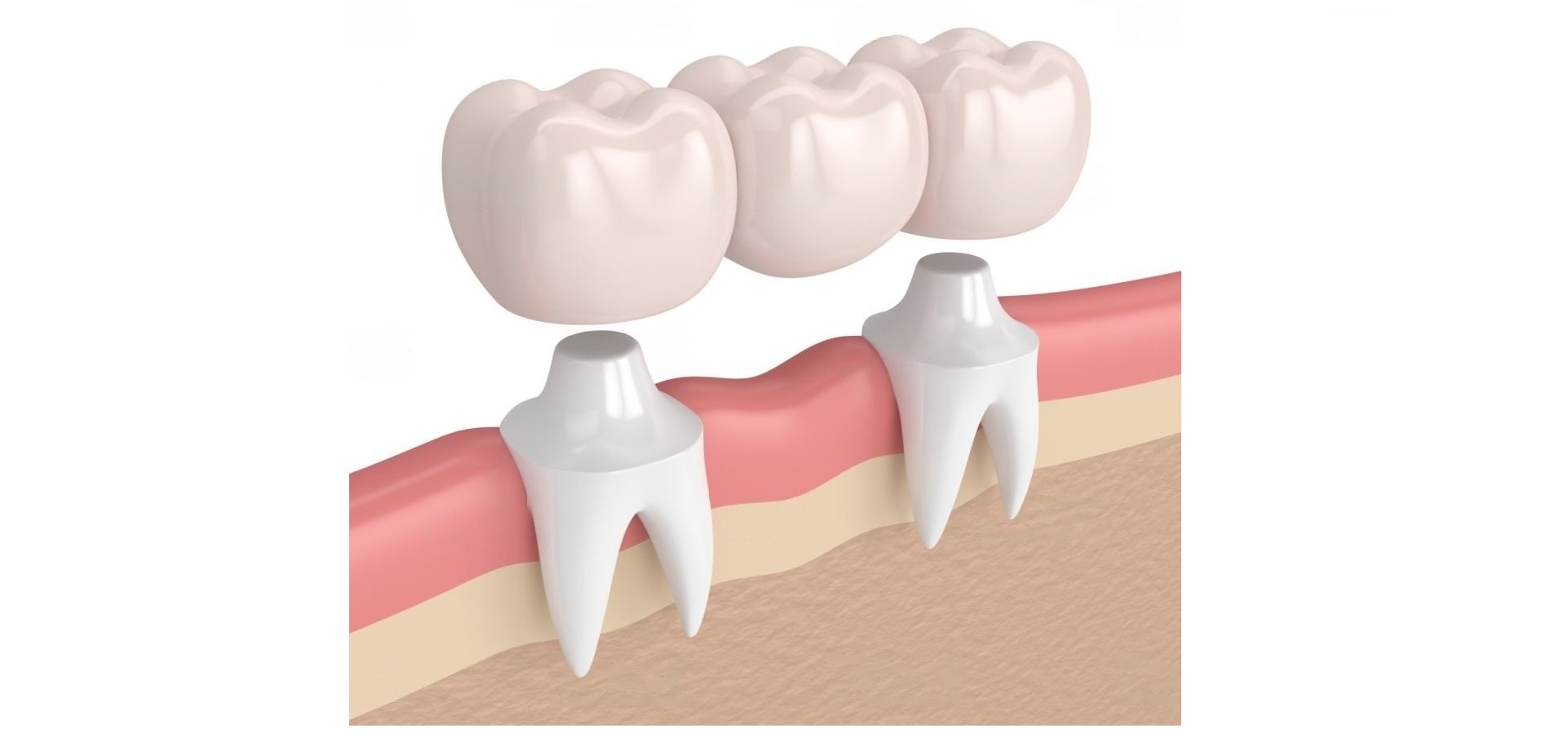
Dental Bridges
What is a dental bridge procedure?
A dental bridge permanently replaces missing teeth with false teeth. The bridge is attached to the teeth on either side of the gap. Bridges are usually made of porcelain or metal, a mixture of the 2, or zirconia. They are fixed in place and, for some people, are an alternative to dentures.
When might you need a dental bridge?
You might need a dental bridge if you have a missing tooth or teeth and have healthy teeth on either side of the gap left by the missing teeth.
What happens during a dental bridge procedure?
First, the dentist will examine the mouth and ensure any tooth decay or gum disease is treated. They may take an x-ray and use equipment to take measurements of the teeth and mouth.
The dentist will usually file down healthy teeth to prepare the dental
bridge.
You might be given a temporary bridge while waiting for your permanent
bridge to be ready. If so, that is
taken out once your permanent bridge has been prepared.
The permanent bridge is put in place when ready, and usually attached to the
surrounding healthy teeth
with dental cement. Or the dentist might anchor the bridge with a dental
implant, which is surgically
placed in the jaw. The dentist will need to check if dental implants are
suitable for you.
How do you care for your dental bridge?
You’ll need to brush your bridge with fluoride toothpaste and floss, as is usually recommended for natural teeth. Regular visits to your dentist are also important.
What are the benefits and risks of a dental bridge procedure?
Dental bridges can help restore the smile and avoid someone feeling self-conscious about having missing teeth. Filling in the gap left by missing teeth is also important because, if the gap is not filled, the surrounding teeth might lean into the gap over time and change the way a person bites.
Bridges can last for many years if they are cared for properly. However, they can fail, usually due to decay of the natural teeth next to them, or failure of the cement.
What are the alternatives to dental bridges?
The main alternative to a dental bridge is using removable false teeth, known as a partial denture, which you can take out to clean. Another alternative is a dental implant.
Implants
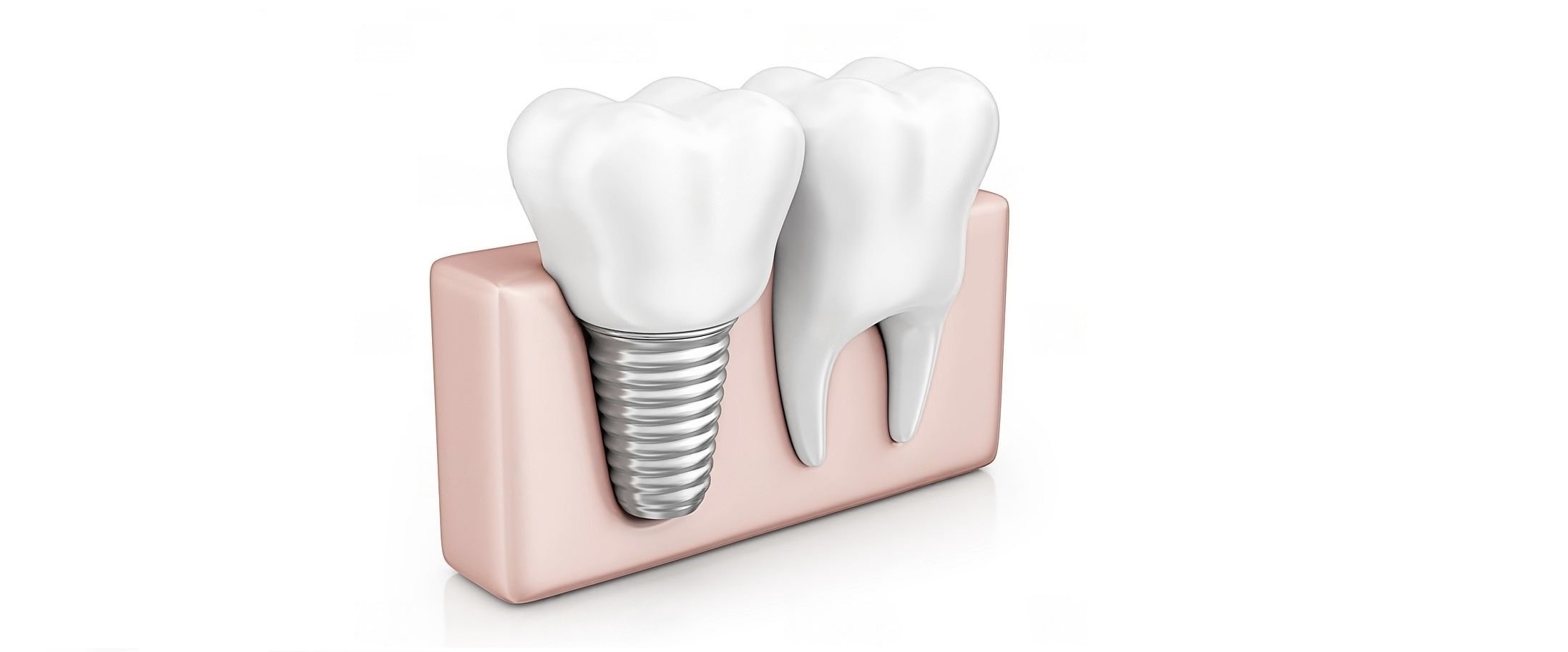
What is a dental implant procedure?
A dental implant procedure is part of a dental operation to replace a missing tooth. Unlike dentures, which are false teeth that you can easily remove, dental implants are placed in the jawbone in a series of minor operations.
What are dental implants?
A dental implant is a piece of titanium or other materials that looks like a screw. It is put into the jaw where the missing tooth’s roots were. Over time, bone grows around the implant, which helps to hold it in place.
An artificial tooth, or crown, is then attached to the metal to fill in the
gap left by the missing tooth. The
crown is specially made to look like the other teeth in size, shape and
colour.
Dental implants can also be used to hold a dental bridge or
dentures in place.
When might a dental implant be needed?
If you have one or more missing teeth, a dental implant might be a
suitable option if you:
have a fully grown, healthy jawbone
don’t have gum disease
don’t have conditions that affect bone healing
Your dentist will discuss with you whether a dental implant procedure is
suitable for you.
What happens during a dental implant procedure?
A dental implant is usually done in stages over a few months, with a series of minor operations and tests.
First, scans and x-rays are done to give the dentist a very clear picture of where to place the implant.
The dental implant is fitted into the jawbone in a minor operation. You will usually be given an anaesthetic so that you don’t feel pain during the surgery.
In a few months, the bone grows around the dental implant.
Once the implant is stable, the dentist will create a foundation for the new tooth or teeth.
Sometime later, the dentist will take a mould of the mouth to make the artificial tooth or teeth.
Finally, the artificial tooth or teeth are screwed or cemented into the foundation.
It’s a slow process, with quite a few visits to the dentist and possibly some trips to have scans or x-rays.
Denture and partial plates:
What are dentures?
Dentures are false teeth that are worn to replace missing teeth. If you have missing teeth, wearing dentures can make eating and speaking easier. It can also avoid a loss of confidence in the way you look dentures may be immediate or delay.
When might you need dentures?
If you have missing teeth, your dentist might speak to you about getting dentures fitted. Dentures are specially made to fit your mouth.
There are 4 main types of dentures:
A full denture rests on the gum and replaces all the teeth on the upper or lower jaw, or both
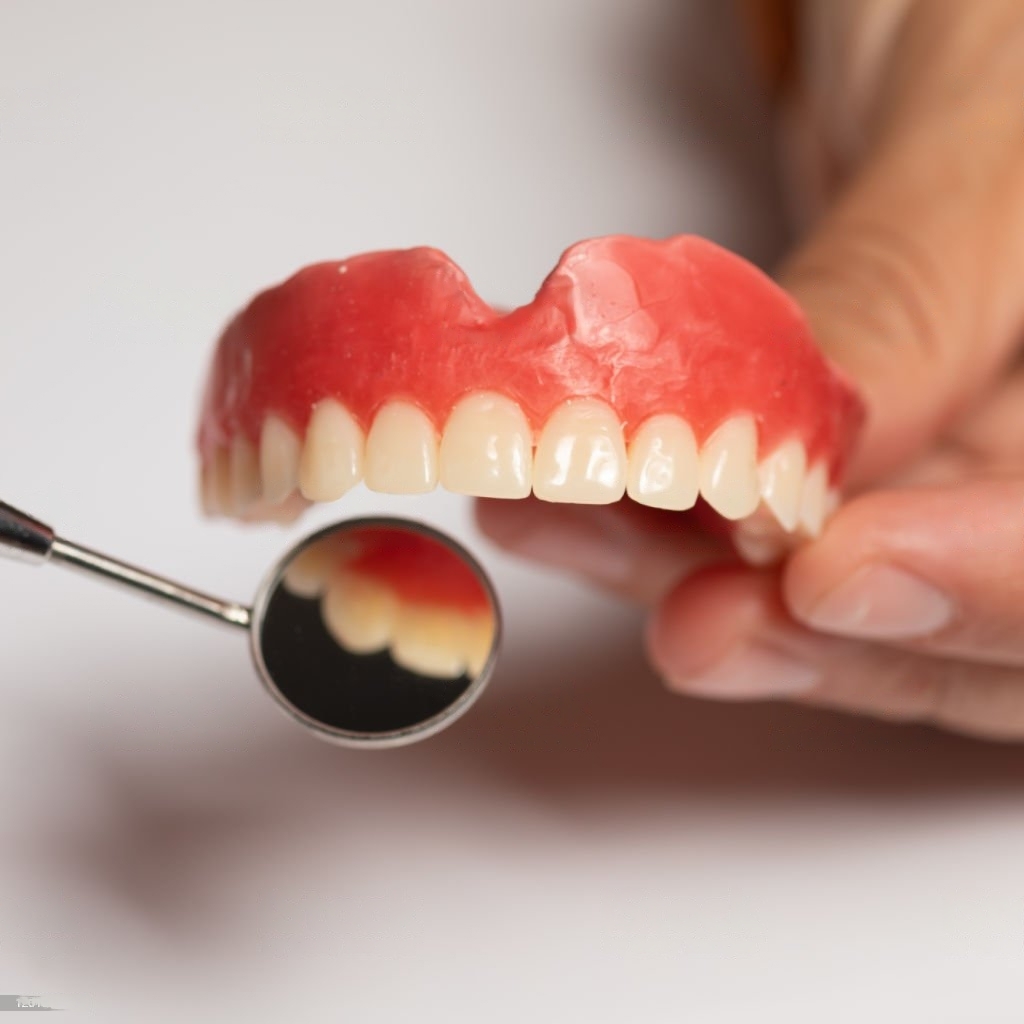
A partial denture replaces some teeth and is held in place by clasps around the remaining teeth.

An implant-retained denture replaces one or more teeth and is fitted through implants in the jaw.
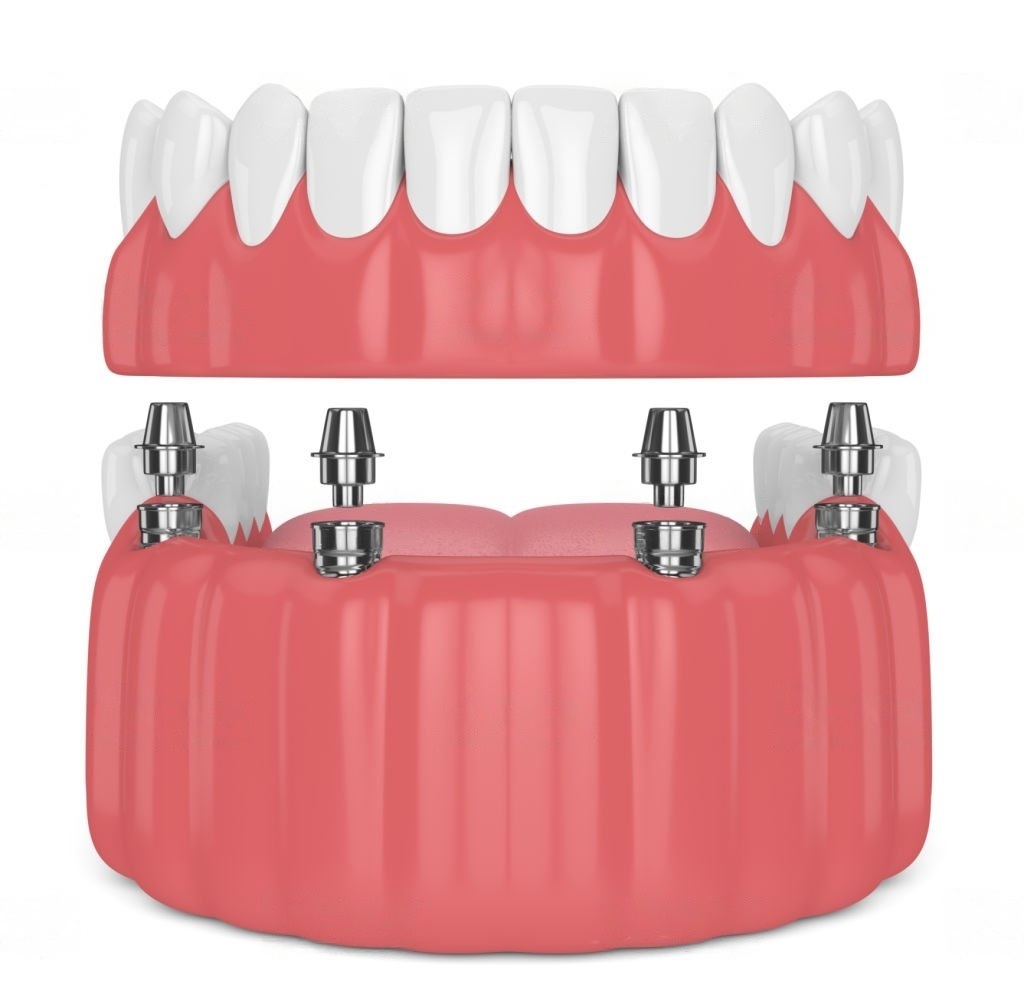
An overdenture/telescopic denture replaces teeth and is fitted over your own remaining teeth, normally the canines.
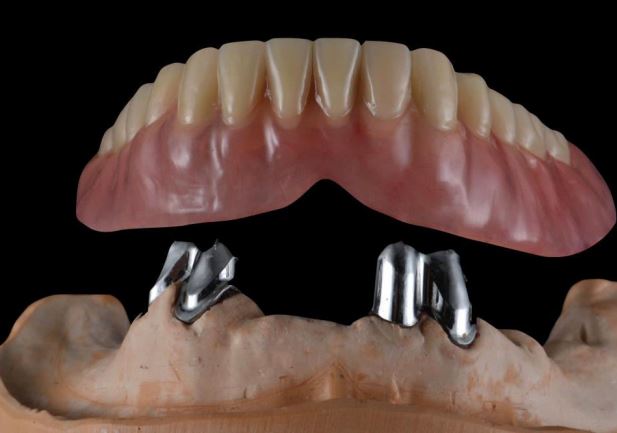
What happens during a denture fitting?
If you’re having your teeth removed, you might choose to have dentures inserted on the same day. This is called an immediate denture. You may need frequent adjustments as your gums heal.
The dentist might ask you if you would wait a few months before getting dentures. This allows your gums to heal so you won’t need as much adjustment once the dentures are in place.
Most people take a few months to adjust to wearing a new set of dentures. They may feel awkward or loose at first. You might feel irritation or soreness. You might have more saliva than normal. Make sure you see your dentist if your mouth is sore, or if you have bleeding gums, swelling or ulcers. They may need to adjust your dentures.
Scale & Polish
Regular hygiene sessions are important for good oral health. To keep your gums in optimum condition, it is advised to have a simple ‘Scale and Polish’ every 6 months at least. We believe the best way to achieve a happy, healthy smile is by regular dental appointments and regular oral hygiene appointments with a Scale and Polish cleaning session.
If your teeth have staining from smoking, tea, coffee and red wine, book in for an EMS air Flow stain removing session as part of your hygiene appointment with us.
Gum Disease/Bleeding Gums
Healthy gums are firm and fit snugly around teeth. The color of healthy gums can vary. They may range from light pink in some people to dark pink and brown in others.
Symptoms of periodontitis can include:
Swollen or puffy gums.
Bright red, dark red or dark purple gums.
Gums that feel tender when touched.
Gums that bleed easily.
A toothbrush that looks pink after brushing your teeth.
Spitting out blood when brushing or flossing your teeth.
Bad breath that won't go away.
Pus between your teeth and gums.
Loose teeth or loss of teeth.
Painful chewing.
New spaces that develop between your teeth that look like black triangles.
Gums that pull away from your teeth, making your teeth look longer than
usual, called receding gums.
A change in the way your teeth fit together when you bite.
Laser Gum Treatment:
Laser Dentistry
Laser dental treatment of gum disease. Laser treatment for periodontal disease commonly called gum disease kills the bad bugs and assists with tissue healing and regeneration which is often an effective treatment for this disease as a part of preventive dental care. This technique can improve the health of the gums and may prevent or delay the loss of teeth due to periodontal disease. If you have been diagnosed with periodontal or gum disease, we can treat this disease using the laser technique.
